
- Haters Gonna Hate. And Post. A Lot. You can find anything on the internet. Anything. If you want someone to validate your distaste for cute, cuddly, perfect Cocker Spaniel puppies, just Google it. You’ll probably find an article called “20 Things I Hate About Cute, Cuddly, Perfect Cocker Spaniel Puppies” in about 2.2 seconds. It will be full of compelling reasons to hate puppies and, if you weren’t a puppy hater before, by the end of the article you’ll certainly be considering it. It’s easy to find both sides of any argument on the internet. And it’s even easier to share said argument with 500 of your closest friends. Most of the time, the articles are well written and authoritative. Most of the time, they are nothing more than opinion pieces written by someone who lacks the credentials to have an actual opinion. (Case in point: former Playboy model Jenny McCarthy. Yes, I went there.) Harsh, I know, but true. Admit it.
- Haters Wanna Benefit from Everyone Else. Haters be like “I got Herd Immunity.” Aww, nah. Herd immunity is like that lane on the interstate that’s closed 500 feet ahead. There’s always that one guy who drives up the lane and cuts in at the last second, causing all the cars behind him to have to slow down. Dude. It’s 7:50 on Monday morning. Everyone is running late. You are no more important than anyone else on the road right now. Notable exceptions are as follows (in no particular order):
- The pregnant woman in active labor, extra points if the baby is crowning. Negative points if the woman is driving herself—that’s just all kinds of dangerous.
- Any emergency vehicles (this is an obvious one), especially if they are going to fix the problem that got the lane closed to begin with.
- The unfortunate sufferer of food poisoning, viral gastroenteritis, or even an especially bad flare-up of IBS.
- The person who will suffer serious consequences if they are late. This category is on the honor system. You usually know deep down if your situation justifies trumping everyone else on the road. Examples include those going to a job interview, an important meeting, his or her own wedding (e.g. the bride or groom – everyone else in the wedding party is going to have to roll in late).
But I digress. Herd immunity, where enough people are immune that an outbreak doesn’t occur in the first place, is to be enjoyed only by those who can’t safely get vaccines. I’m talking about the immune-compromised, the very young, the seriously allergic, the pregnant (in some cases, not all). Otherwise, it just doesn’t work. The goal vaccination rate for the total population is 90-95% for herd immunity to work. We got a first-hand look at this breakdown in herd immunity with the 2015 outbreak of measles beginning in California. It can be quite scary for those of us with children too young to be vaccinated.
- Haters Don’t Really Get It. They be like “Vaccines are bad for you.” This is actually a three part argument.

3a. Haters say vaccines give you the infection you’re trying to avoid. We’ve all heard some iteration of the following: “I never got the flu until the one year I actually got the flu vaccine.” Seems like a compelling argument. Either the vaccine gave your friend the flu or, at the very least, it didn’t protect him against it. Here is an example of similar logic: I got in a car accident while wearing my seatbelt and suffered an injury. Oh man, must have been because you had the seatbelt on. Or at the very least, the seatbelt didn’t protect you. Or what if the seatbelt actually caused the accident?
Everyone reading this can appreciate the flawed logic in the above statement. There is no cause and effect. Just coincidence and perhaps some unrealistic expectations. And while the seatbelt may not have kept you from getting injured, it may have just saved your life. The flu vaccine often keeps one from contracting the flu in the first place, but it also lessens the severity of the illness in those who get infected despite receiving the vaccine. In the case of the flu, this protection is often as important as the prevention aspect. Some years, despite their best efforts, the vaccine developers don’t get the match quite right because of mutations that occur after the strains are chosen for the vaccine.
And as for whether the flu shot causes the flu, it doesn’t. It just doesn’t. While the intranasal form of the vaccine has a theoretical risk of causing a flu infection (because it is an altered form of the live virus and therefore has the afore-mentioned propensity for mutation), the injection is a dead virus. And viruses are not zombies. They do not come back alive for one last hurrah terrorizing humans.
There are over 300 million people in this country. Everyone has heard a story from someone about the flu shot “making them sick,” but in the end it’s all about odds. They were going to get sick, anyway. It’s just coincidence. And if it was at least two weeks after the shot, then they can be grateful because it could have been a lot worse.
3b. They say vaccines cause autism: This is the argument that’s gotten the most press recently. Autism rates have increased at alarming rates over the past two decades. Over the same time period, the number of recommended vaccines has increased. Again, correlation does not prove causation. A lot has changed in that time frame. One notable change was in the criteria used to diagnose autism. Another was in provider awareness of the disorder. These two things don’t actually change the prevalence of a disease, they just change the perceived prevalence.
A now infamous study by Andrew Wakefield claimed to show a connection between vaccines (specifically, the MMR vaccine) and autism. Usually, doctors evaluate the quality of a study based on its ability to prove its hypothesis by how well it was designed: were there enough patients? Was it randomized? Was all potential bias removed? You get the point.

However, this study failed on several more serious counts. The study authors began the study in an attempt to provide a basis for a lawsuit to win money. That’s just a bad start. Then, patients were recruited by an anti-vaccine group. This is an example of selection bias. Then, medical records were intentionally falsified. Wait, isn’t that?…Why yes. Yes it is quite illegal. It’s called fraud. And that’s why the article was retracted by the original journal in which it was published.
But people still want to trust lying, cheating Andrew Wakefield over the doctor they have chosen to care for their child in all other aspects. The doctor who has taken a Hippocratic Oath to “first, do no harm.” The doctor who, dollars to donuts, has vaccinated the crap out of his or her own children. Yes, there are bad people in medicine. Just like there are bad people in every profession. But the law of probabilities would argue that we can’t all be bad. If it’s true that the entire medical community can’t be trusted, then society has much bigger problems than anyone realized.
As a side note, the preservative thimerosal has also received a bad rap lately because it contains mercury in very small amounts. Again, there has been no literature to prove a negative effect of this, but as a precautionary measure, the AAP/USPHS recommended removing thimerosal from several vaccines to reduce the cumulative exposure over time. So to recap, the regulatory boards recognized a potential health risk, albeit one that had not been proven, and decided to err on the side of caution and eliminate the possibility of this preventable risk.
3c. Haters say vaccines overwhelm the immune system: Some worry that children are exposed to too many antigens at once, that it weakens the immune system or causes it to be oversensitive and lead to illnesses such as autoimmune conditions or asthma. Again, there is just no evidence to support this.
Anyone who knows me knows I am a huge proponent of letting my children eat dirt, lick the floor, etc. I wholeheartedly believe we shouldn’t follow our children around, sterilizing each surface they come into contact with. There is a benefit to challenging their little immune systems so they aren’t completely taken off guard when they finally come into contact with a more dangerous bacteria or virus.
But a vaccine is a challenge to the immune system in the purest sense. It simulates a “first” infection so that it will then respond much more quickly if exposed a “second” time. Scientists figured out this is the way immunity works and used it to our advantage. Science is awesome that way.

And while I do believe in encouraging natural exposure to infections at an early age, if given the opportunity to test this theory with potentially fatal illnesses in my children, my answer will always be, “Thanks, but no thanks.” I’ve seen enough to know better. In my opinion, that would be akin to letting child jump off a 100 foot bridge to teach him not to jump off 100 foot bridges in the future.
If you’re still not convinced, I’ll share this interesting fact: with ongoing vaccine development, the number of antigens children are exposed to today is about 10% of what it was in 1980.
- Haters haven’t learned from the past. They think vaccines are irrelevant. Who’s scared of polio, anyway? Do you even know anyone who has polio? Exactly. But let me assure you, people used to be plenty scared of polio. And the measles, mumps, rubella…I could go on, but in the interest of time I won’t. Everyone has a grandparent or great-grandparent who had a sibling or child die when he or she was a child. The cause of death for most of these children, if it didn’t occur during childbirth, was usually some sort of infection. In fact, the leading causes of child mortality in 1900 were infectious diseases—a whopping 61.6%. In 1998, death attributable to infectious disease was only 2%. During that same time period, the absolute death rate plummeted from >3% to <0.2%, reflecting an even greater absolute (total) reduction in infectious diseases. While this decline reflects many changes during that time period including improved antiseptic techniques, antibiotic development and cleaner living conditions, vaccines played a major role in this shift.
And, lest we forget that not all vaccine-preventable infections end in death, other potential consequences include but are not limited to hearing loss, increased susceptibility to other infections, encephalitis, pneumonia, ear infections, bronchitis, dehydration, vomiting, difficulty breathing…it’s a little reminiscent of the disclaimer at the end of a Viagra commercial, isn’t it?
- Haters say doctors just want to give a bunch of medications.

Vaccines are actually a prime example of preventative medicine. Yes, they come in a vial. But when used correctly, they significantly lower the need for hospitalizations, antibiotics, and other therapies. Like a healthy diet and lifestyle, in an ideal world, vaccines should lead to fewer doctor visits and interventions.
In conclusion, medicine is not black and white, as much as we would often like it to be. There are times when we have to choose the best for our patients based on a risk-benefit analysis. And based on the information available, the benefits of getting vaccinated far, far outweigh the risks. And so we will carry on, spending extra time educating our patients, cringing when we hear of the next outbreak that could have been prevented, and praying for the children and the parents of the children who fall ill or even die from a preventable illness.
Disclaimer: The opinions expressed in this blog post are not meant to offend, but to reinforce proven information in an entertaining way. The facts presented in this blog post are facts.
The following resources were referred to during the preparation of this post:
CDC.gov
Deer B. How the case against the MMR vaccine was fixed. BMJ 2011; 342:c5347. (An interesting article by the investigative reporter who uncovered Andrew Wakefield, et al., had committed fraud.)
DeStefano F, Price CS, Weintraub ES. Increasing exposure to antibody-stimulating proteins and polysaccharides in vaccines is not associated with risk of autism. J Pediatr 2013; 163:561.
Guyer B, Freedman MA, Strobino DM, Sondik EJ. Annual summary of vital statistics: trends in the health of Americans during the 20th century. Pediatrics. 2000 Dec; 106(6): 1307-17.
Iqbal S, Barile JP, Thompson WW, DeStefano F. Number of antigens in early childhood vaccines and neuropsychological outcomes at age 7-10 years. Pharmacoepidemiol Drug Saf 2013; 22:1263.
Lieberman JM. Myths regarding immunization. In: An Ounce of Prevention: Communicating the Benefits and Risks of Vaccines to Parents. Infectious Diseases in Children. Slack Incorporated, Thorofare, NJ 2003. P.6.
Lyren A, Leonard E. Vaccine refusal: issues for the primary care physician. Clin Pediatr (Phila) 2006; 45:399.
Offit PA, Quarles J, Gerber MA, et al. Addressing parents’ concerns: do multiple vaccines overwhelm or weaken the infant’s immune system? Pediatrics 2002; 109:124.
Vaccines.gov
Wakefield AJ, Murch SH, Anthony A, et al. Ileal-lymphoid-nodular hyperplasia, non-specific colitis, and pervasive developmental disorder in children. Lancet 1998; 351:637. (The original article “linking” vaccines and autism which was later retracted.)
*There have been many large studies and reviews showing no link between the MMR vaccine and autism, too many to list here. If you are interested, please contact me for a comprehensive list.





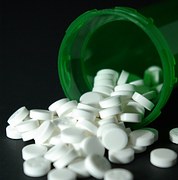
 If doctors are resistant to prescribing pain medications, it’s not because we want to maintain some sort of control or power over the situation. It’s the easiest thing in the world to write a prescription, and to feel like a hero for it, but that’s not doctoring. Doctoring is talking to your patient, listening to their complaints, and deciding on a treatment plan that has the best chance of helping them without harming them. When we are faced with data that shows no long-term benefit to opioid medications, and then we see the potential harm they can cause, we do not take the decision to prescribe these medications lightly. That is not to say that I will never, ever prescribe opioids ever again. But each and every time I do, I think long and hard about it. And I hope my patients can appreciate that about me, because it’s unlikely to change.
If doctors are resistant to prescribing pain medications, it’s not because we want to maintain some sort of control or power over the situation. It’s the easiest thing in the world to write a prescription, and to feel like a hero for it, but that’s not doctoring. Doctoring is talking to your patient, listening to their complaints, and deciding on a treatment plan that has the best chance of helping them without harming them. When we are faced with data that shows no long-term benefit to opioid medications, and then we see the potential harm they can cause, we do not take the decision to prescribe these medications lightly. That is not to say that I will never, ever prescribe opioids ever again. But each and every time I do, I think long and hard about it. And I hope my patients can appreciate that about me, because it’s unlikely to change. accurately, reduce the perception of pain. Pain causes an increase in certain neurotransmitters in the brain. Just like depression, managing it is often an issue of modulating the neurotransmitters to alter the experience of pain. Actually, a few antidepressants have been found to be effective in the management of certain chronic pain conditions for this very reason.
accurately, reduce the perception of pain. Pain causes an increase in certain neurotransmitters in the brain. Just like depression, managing it is often an issue of modulating the neurotransmitters to alter the experience of pain. Actually, a few antidepressants have been found to be effective in the management of certain chronic pain conditions for this very reason. Happily, there are many other options available to us for the treatment of pain. There are non-pharmacologic treatments such as physical therapy, yoga, massage therapy, meditation, and multiple other modalities. On the medication front, we have anti-inflammatory medications, anticonvulsants, antidepressants, muscle relaxers, topical medications, and anti-anxiety medications. There is also the option of regional analgesia, which includes a variety of procedures that can be performed to focus in on a specific painful area. Depending on the type of pain a patient is having, one or more of the above options is likely to be more beneficial than opioids and will almost certainly result in improved function and lifestyle.
Happily, there are many other options available to us for the treatment of pain. There are non-pharmacologic treatments such as physical therapy, yoga, massage therapy, meditation, and multiple other modalities. On the medication front, we have anti-inflammatory medications, anticonvulsants, antidepressants, muscle relaxers, topical medications, and anti-anxiety medications. There is also the option of regional analgesia, which includes a variety of procedures that can be performed to focus in on a specific painful area. Depending on the type of pain a patient is having, one or more of the above options is likely to be more beneficial than opioids and will almost certainly result in improved function and lifestyle.
 harm someone by prescribing opioids. That is why we can seem so unnecessarily cautious. That is why we weigh the options so carefully. That is why we have pain contracts and rules. If your doctor is cautious about prescribing opioids, it usually means they care.
harm someone by prescribing opioids. That is why we can seem so unnecessarily cautious. That is why we weigh the options so carefully. That is why we have pain contracts and rules. If your doctor is cautious about prescribing opioids, it usually means they care.
 Pain as the fifth vital sign. In an effort to standardize and improve pain treatment for patients, a national initiative called Pain as the 5th Vital Sign (P5VS) was rolled out in the late nineties. The well-meaning folks who began this initiative were trying to improve the health and well-being of the over 34 million patients in this country that suffer from chronic pain. Unfortunately, a study published in the Journal of General Internal Medicine in 2006 (
Pain as the fifth vital sign. In an effort to standardize and improve pain treatment for patients, a national initiative called Pain as the 5th Vital Sign (P5VS) was rolled out in the late nineties. The well-meaning folks who began this initiative were trying to improve the health and well-being of the over 34 million patients in this country that suffer from chronic pain. Unfortunately, a study published in the Journal of General Internal Medicine in 2006 (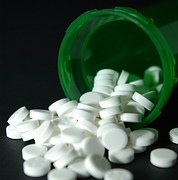 1996. It was heavily marketed, both to consumers directly and to doctors. It was supposed to be the best thing to happen to chronic pain in the history of chronic pain (i.e. civilization). We were told the chances of addition were miniscule because of the time-release formulation, and the potential benefits were unimaginable. The pharmaceutical company that made OxyContin (getting a new patent for a drug that had been around for the better part of a century) did a phenomenal job of getting their product out there, and doctors who hesitated to prescribe it were vilified. It was a veritable love fest, reminiscent of an Oprah Winfrey episode. “You get OxyContin! You get OxyContin! Everyone gets OxyContin!”
1996. It was heavily marketed, both to consumers directly and to doctors. It was supposed to be the best thing to happen to chronic pain in the history of chronic pain (i.e. civilization). We were told the chances of addition were miniscule because of the time-release formulation, and the potential benefits were unimaginable. The pharmaceutical company that made OxyContin (getting a new patent for a drug that had been around for the better part of a century) did a phenomenal job of getting their product out there, and doctors who hesitated to prescribe it were vilified. It was a veritable love fest, reminiscent of an Oprah Winfrey episode. “You get OxyContin! You get OxyContin! Everyone gets OxyContin!” example, sometimes we must tell a patient that their weight is negatively affecting their health. Or their smoking. Or any other number of bad habits. It’s the right thing to do. If we didn’t do it, we would be doing our patients a disservice. But it’s still not always nice for patients to hear. It doesn’t necessarily give them a warm, fuzzy feeling when leaving our office, nor does it make them want to send their friends and family to us to receive the same kind of tough love.
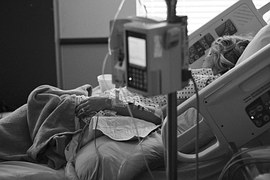
example, sometimes we must tell a patient that their weight is negatively affecting their health. Or their smoking. Or any other number of bad habits. It’s the right thing to do. If we didn’t do it, we would be doing our patients a disservice. But it’s still not always nice for patients to hear. It doesn’t necessarily give them a warm, fuzzy feeling when leaving our office, nor does it make them want to send their friends and family to us to receive the same kind of tough love. these medications, but we also take a significant risk each time we prescribe them. We risk our patient developing a dependence or addiction, we risk the medications being diverted or abused, we risk saddling patients with side effects that can be worse than their primary complaint (such as severe constipation and even narcotic bowel syndrome), and we risk someone dying from an overdose of medications we prescribed. Not only are we then “doing harm,” which we took an oath against, but we could even possibly be implicated in someone’s death. I’m sure no one’s forgotten Conrad Murray, the personal physician of Michael Jackson, who was convicted of involuntary manslaughter after Jackson’s death. That’s an extreme case, sure, but it can happen.
these medications, but we also take a significant risk each time we prescribe them. We risk our patient developing a dependence or addiction, we risk the medications being diverted or abused, we risk saddling patients with side effects that can be worse than their primary complaint (such as severe constipation and even narcotic bowel syndrome), and we risk someone dying from an overdose of medications we prescribed. Not only are we then “doing harm,” which we took an oath against, but we could even possibly be implicated in someone’s death. I’m sure no one’s forgotten Conrad Murray, the personal physician of Michael Jackson, who was convicted of involuntary manslaughter after Jackson’s death. That’s an extreme case, sure, but it can happen.









 1. Don’t Lie. It doesn’t do you any favors to be untruthful to your doctor. Unless you tell your doctor something along the lines of “I want to kill my spouse and I have a loaded gun in my car which I am going to use for said crime,” whatever you say during your visit is completely confidential. And certain things can actually factor into medical decision-making. For example, a thirty-year-old who complains of chest pain is very unlikely to be having a heart attack, unless…(wait for it)…he’s been doing lines of coke. Then, a big ol’ heart attack is back on the differential. And heart attacks are treated a little bit differently than your run of the mill musculoskeletal chest pain.
1. Don’t Lie. It doesn’t do you any favors to be untruthful to your doctor. Unless you tell your doctor something along the lines of “I want to kill my spouse and I have a loaded gun in my car which I am going to use for said crime,” whatever you say during your visit is completely confidential. And certain things can actually factor into medical decision-making. For example, a thirty-year-old who complains of chest pain is very unlikely to be having a heart attack, unless…(wait for it)…he’s been doing lines of coke. Then, a big ol’ heart attack is back on the differential. And heart attacks are treated a little bit differently than your run of the mill musculoskeletal chest pain. time he walks in the exam room. I’m just talking about extending the same respect you give to the people who bag your groceries and cut your hair. Respect them when you think they look young (they have been through years of training and probably still remember most of it), respect them when they say they don’t know (which is much better than pretending they know when they don’t), and respect them when they don’t order every test known to man (they probably have a good knowledge base and/or physical exam skills and don’t require the extra reassurance from unnecessary and sometimes harmful tests). You don’t have to trust them blindly, just respect them.
time he walks in the exam room. I’m just talking about extending the same respect you give to the people who bag your groceries and cut your hair. Respect them when you think they look young (they have been through years of training and probably still remember most of it), respect them when they say they don’t know (which is much better than pretending they know when they don’t), and respect them when they don’t order every test known to man (they probably have a good knowledge base and/or physical exam skills and don’t require the extra reassurance from unnecessary and sometimes harmful tests). You don’t have to trust them blindly, just respect them.
 the possibility of resistance (that’s why you need to take every single pill in the bottle, even when you’re feeling better). This is relevant because bacteria are developing resistance faster than we are able to develop new antibiotics, therefore resulting in the “superbugs” you’ve heard so much about. By and large, these are just “regular bugs who are now too smart for our usual defenses”—but that doesn’t have quite the same ring to it, does it? Anyway, all that to say when your doctor doesn’t want to prescribe antibiotics she’s not trying to punish you or be withholding. She’s trying to practice responsible medicine. Please, let her do her job.
the possibility of resistance (that’s why you need to take every single pill in the bottle, even when you’re feeling better). This is relevant because bacteria are developing resistance faster than we are able to develop new antibiotics, therefore resulting in the “superbugs” you’ve heard so much about. By and large, these are just “regular bugs who are now too smart for our usual defenses”—but that doesn’t have quite the same ring to it, does it? Anyway, all that to say when your doctor doesn’t want to prescribe antibiotics she’s not trying to punish you or be withholding. She’s trying to practice responsible medicine. Please, let her do her job. and down their arms. They often have good jobs, families, and responsibilities. They have a lot to lose. It has much less to do with willpower or a moral compass than you might think, and more to do with a genetic predisposition (that a patient wouldn’t even know they had). I’ve heard the story before, and I’ll hear it again, of a person who lost everything after a seemingly innocent prescription for Percocet totally derailed their life.
and down their arms. They often have good jobs, families, and responsibilities. They have a lot to lose. It has much less to do with willpower or a moral compass than you might think, and more to do with a genetic predisposition (that a patient wouldn’t even know they had). I’ve heard the story before, and I’ll hear it again, of a person who lost everything after a seemingly innocent prescription for Percocet totally derailed their life. and controlling your blood sugar. Patients who take ownership of their health often stay out of the hospital and even their doctor’s offices for the most part. Practicing a healthy lifestyle significantly limits the amount of healthcare and medications you have to r
and controlling your blood sugar. Patients who take ownership of their health often stay out of the hospital and even their doctor’s offices for the most part. Practicing a healthy lifestyle significantly limits the amount of healthcare and medications you have to r eceive over your lifetime. We know that high blood pressure and cholesterol leads to strokes and heart attacks;
eceive over your lifetime. We know that high blood pressure and cholesterol leads to strokes and heart attacks; You go to a doctor because they are trained to take care of the human body during times of illness. You may not have experience with a certain ailment, but you can rest assured that your doctor almost certainly does (and they should tell you if they don’t). Most of the time, their prescribed course of therapy—while it could seem strange or inconvenient to you—is a tried and true, common, safe, and effective treatment.
You go to a doctor because they are trained to take care of the human body during times of illness. You may not have experience with a certain ailment, but you can rest assured that your doctor almost certainly does (and they should tell you if they don’t). Most of the time, their prescribed course of therapy—while it could seem strange or inconvenient to you—is a tried and true, common, safe, and effective treatment.



 ur kids’ teachers to shield them from that reality? Why would we want them to? I want my kids to strive for excellence, not mediocrity. I want them to work for what they get, not expect a free ride. Lately, high school seems to be considered fluff. A means to an
ur kids’ teachers to shield them from that reality? Why would we want them to? I want my kids to strive for excellence, not mediocrity. I want them to work for what they get, not expect a free ride. Lately, high school seems to be considered fluff. A means to an






 hiding inside that little two and a half year old body. President of the United States or CEO of a Fortune 500 company or amazingly talented artist or professional athlete. He’ll still get into a decent college. Have friends. Be happy.
hiding inside that little two and a half year old body. President of the United States or CEO of a Fortune 500 company or amazingly talented artist or professional athlete. He’ll still get into a decent college. Have friends. Be happy. d up equal to or even ahead of them by the end of the school year.
d up equal to or even ahead of them by the end of the school year.




 of thinking about things, who figures things out and is always trying something new. The most successful businessmen, doctors, researchers, and engineers are people who tackle old problems in new ways. This kid of gift is fostered early on by allowing kids to figure things out on their own—or with friends—instead of jamming it down their throats against their will. Play has been shown to benefit kids by increasing conceptual knowledge, problem-solving, creativity, skills required in STEM (Science, Technology, Engineering and Math) fields, language and literacy, and self control.
of thinking about things, who figures things out and is always trying something new. The most successful businessmen, doctors, researchers, and engineers are people who tackle old problems in new ways. This kid of gift is fostered early on by allowing kids to figure things out on their own—or with friends—instead of jamming it down their throats against their will. Play has been shown to benefit kids by increasing conceptual knowledge, problem-solving, creativity, skills required in STEM (Science, Technology, Engineering and Math) fields, language and literacy, and self control. new things, and figure out what they’re good at and what they enjoy. It also fosters a love for physical activity in whatever form it may take for that child, resulting in a healthier weight and lifestyle. And who knows, if you just sit back and watch, your kid may just tell you he could be the next Wayne Gretzky.
new things, and figure out what they’re good at and what they enjoy. It also fosters a love for physical activity in whatever form it may take for that child, resulting in a healthier weight and lifestyle. And who knows, if you just sit back and watch, your kid may just tell you he could be the next Wayne Gretzky.















